Pharmacogenomic Testing:
What is it and who should get it?

What is Pharmacogenomics or Pharmacogenetics (PGx)?
The science of pharmacogenomics combines pharmacology and genomics to determine how a person’s genes might influence the way he or she responds to medications. Treatments for illness can be influenced by PGx testing.
While PGx testing cannot determine “the perfect drug” for everyone, it provides a clinician with valuable genetic information that helps them make informed decisions after reviewing the patient’s symptoms, previous treatment responses, family history, and treatment goals.
It can provide valuable insight by looking at genes that could impact:
- A person’s body’s ability to metabolise and absorb medicines.
- Medicine sensitivity (which may increase or decrease a person’s risk of medication-related side effects).
- It can be a useful tool for doctors when considering different treatment options or individualising doses to best help the patient.
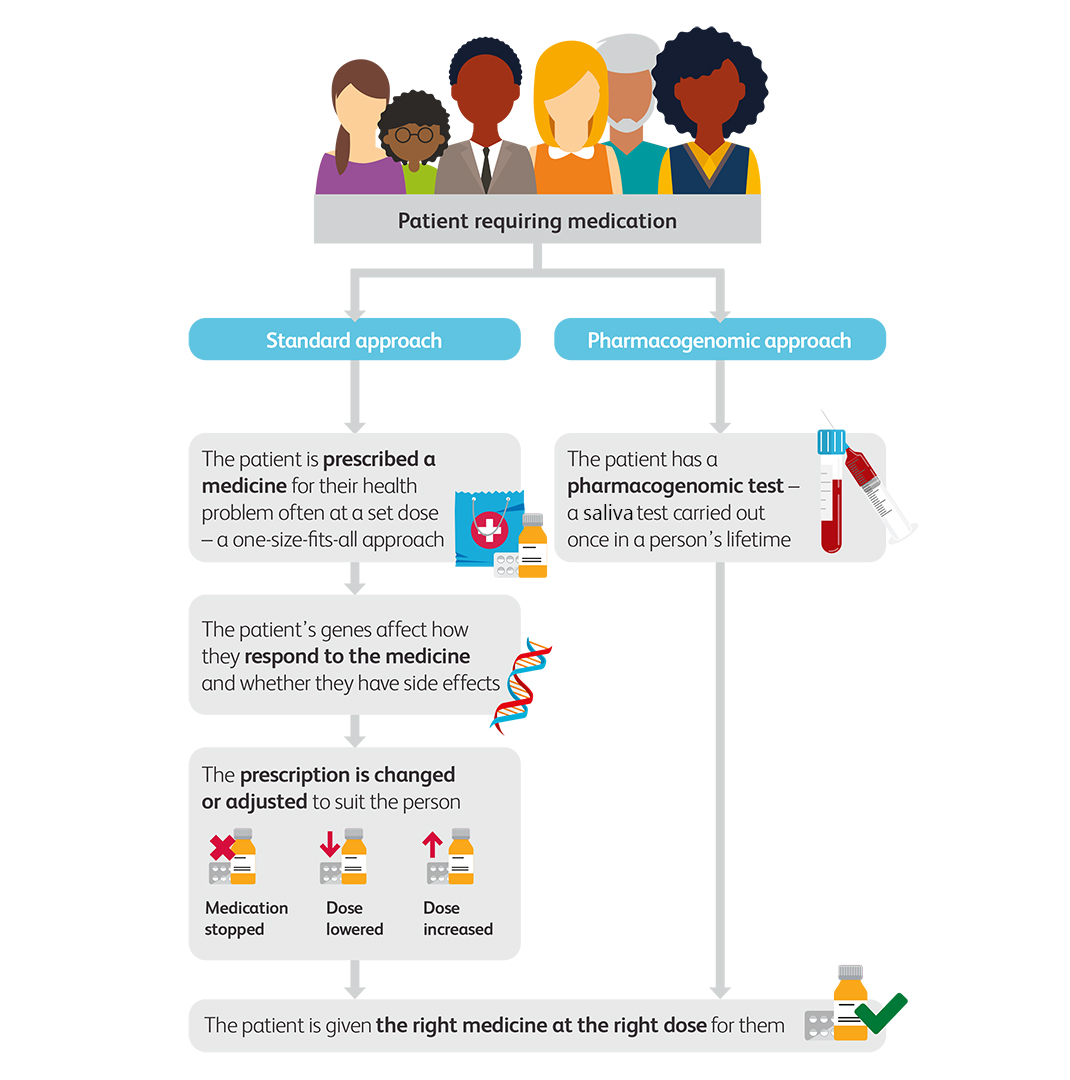
The Evidence Supporting PGx is Growing
Though pharmacogenomic testing (PGx) has been around for several years, there has been some hesitation in the mental health community to widely adopt this practice. The results of this testing may not be fully understood by some clinicians (and they have difficulty explaining the results to their patients) as they consider it “experimental” or “not ready for prime time.”
With the growing popularity of this tool (and the sophistication of the tests by including more genes of interest), accredited healthcare establishments or respected institutions are increasingly acknowledging PGx testing.
For example:
Lord David Prior, the chairman of NHS England, said: “This will revolutionise medicine. Pharmacogenomics “is the future” and “it can now help us to deliver a new, modern personalised healthcare system fit for 2022”.
- In the USA, the Food and Drug Administration has stated, “Pharmacogenomics can play a critical role in identifying responders and non-responders to medicines, avoiding adverse events, and optimizing drug dose.”
- The American Psychiatric Association’s (APA) updated 2020 schizophrenia treatment guidelines recognized that treatment with antipsychotics “can be influenced by genetic differences and metabolic enzyme activity.”
- In a random-effects meta-analysis, (i.e., a study of studies), patients with Major Depressive Disorder tested with PGx were 71% more likely to achieve remission on their medication regimen compared to participants receiving treatment as usual.

Who would benefit most from PGx Testing?
- A patient should be aware that pharmacogenomic testing does not provide clinical insight into the diagnosis of an individual at this time. By PGx testing, a person can optimise their treatment path by finding the right medication and dosage, reducing the need for trial and error. Ideal candidates include:
- A person who is concerned about developing side effects from medicines or who has already experienced significant side effects from medication in the past.
- People with comorbid conditions (co-occurring disorders): Treating one condition alone is challenging. The addition of additional diagnoses can significantly complicate treatment. Additionally, patients with comorbid conditions are often prescribed multiple medications for their different conditions and/or symptoms (increasing the risk of drug interactions).
- A patient’s lifestyle factors, such as coffee consumption or tobacco smoking, may affect drug blood levels and, therefore, drug tolerability.
- Another important aspect of pharmacogenomic testing is that the genes of a person never change, which is important to patients who want to know more about themselves and their biology. Therefore, the results are theoretically valid for life and can be used for alternative conditions (or alternative medicines) as needed in the future.
Genetic testing and genetics have had a far-reaching impact on society and medicine due to the explosion of genetics and genetic testing. Genetic information is becoming increasingly acceptable among people as a way to learn more about their ancestry, disease risks, and-in mental health-related cases, one’s potential response to medication being administered. PGx testing is gaining traction in the mental health field, perhaps at its strongest point in history. There are likely to be more PGx tests used in psychiatry as doctors and patients receive more education, reimbursement is more consistent, and workflow issues are resolved.
At Myogenes our experts have spent years formulating a series of tests which offer you real insights relating to your health such as The Pharmacogenetic Test, The Psychiatric Pharmacogenetic Test, The Hereditary Cancer Test, The Cardiology Test, and The Health & Wellbeing Test.
To speak to one of our advisors today, call us on 020 837 1266 or email info@myogenes.com